Articles
- Page Path
- HOME > Epidemiol Health > Volume 39; 2017 > Article
-
Methods
The unrealized potential: cohort effects and age-period-cohort analysis -
Jongho Heo1
 , Sun-Young Jeon2
, Sun-Young Jeon2 , Chang-Mo Oh3
, Chang-Mo Oh3 , Jongnam Hwang4
, Jongnam Hwang4 , Juhwan Oh1
, Juhwan Oh1 , Youngtae Cho5
, Youngtae Cho5
-
Epidemiol Health 2017;39:e2017056.
DOI: https://doi.org/10.4178/epih.e2017056
Published online: December 5, 2017
1JW LEE Center for Global Medicine, Seoul National University College of Medicine, Seoul, Korea
2Center for Healthcare Policy and Research, University of California Davis, Davis, CA, USA
3Department of Preventive Medicine, Kyung Hee University School of Medicine, Seoul, Korea
4Department of Health Promotion, Daegu University, Daegu, Korea
5Graduate School of Public Health, Seoul National University, Seoul, Korea
- Correspondence: Youngtae Cho Graduate School of Public Health, Seoul National University, 221 Gwanak-ro, Gwanak-gu, Seoul 08826, Korea E-mail: youngtae@snu.ac.kr
• Received: September 18, 2017 • Accepted: October 30, 2017
©2017, Korean Society of Epidemiology
This is an open-access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
- Abstract
- INTRODUCTION
- IDENTIFICATION PROBLEM AND HISTORICAL EVOLUTION OF AGE-PERIOD-COHORT ANALYSIS
- AGE-PERIOD-COHORT ANALYSIS USING AN INTRINSIC ESTIMATOR
- HIERARCHICAL AGE-PERIOD-COHORT ANALYSIS USING CROSS-CLASSIFIED RANDOM EFFECT MODELS
- HIERARCHICAL AGE-PERIOD-COHORT-GROWTH CURVE MODEL USING ACCELERATED LONGITUDINAL PANEL DATA
- CONCLUSION: FUTURE OF AGE-PERIOD-COHORT STUDY IN KOREA
- NOTES
- SUPPLEMENTARY MATERIAL
- REFERENCES
Abstract
- This study aims to provide a systematical introduction of age-period-cohort (APC) analysis to South Korean readers who are unfamiliar with this method (we provide an extended version of this study in Korean). As health data in South Korea has substantially accumulated, population-level studies that explore long-term trends of health status and health inequalities and identify macrosocial determinants of the trends are needed. Analyzing long-term trends requires to discern independent effects of age, period, and cohort using APC analysis. Most existing health and aging literature have used cross-sectional or short-term available panel data to identify age or period effects ignoring cohort effects. This under-use of APC analysis may be attributed to the identification (ID) problem caused by the perfect linear dependency across age, period, and cohort. This study explores recently developed three APC models to address the ID problem and adequately estimate the effects of A-P-C: intrinsic estimator-APC models for tabular age by period data; hierarchical cross-classified random effects models for repeated cross-sectional data; and hierarchical APC-growth curve models for accelerated longitudinal panel data. An analytic exemplar for each model was provided. APC analysis may contribute to identifying biological, historical, and socioeconomic determinants in long-term trends of health status and health inequalities as well as examining Korean’s aging trajectories and temporal trends of period and cohort effects. For designing effective health policies that improve Korean population’s health and reduce health inequalities, it is essential to understand independent effects of the three temporal factors by using the innovative APC models.
- To date, a significant portion of studies on health status or health inequalities in South Korea (hereafter Korea) were cross-sectional studies or studies using short-term accumulated data, which did not consider time lapse. As national-level health data has accumulated during the past decade, it is necessary to examine how population health status and health inequalities change over a longer period, or what are the contributing factors to those changes.
- Age, period, and (birth) cohort are demographic concepts that must be considered in the long-term trend analysis on health-related variables of the population. This study aimed to provide a systematical introduction of age-period-cohort (APC) analysis to Korean readers, in particular, health researchers. The analytical method is used to study independent effects of the three factors on long-term trends of health status and health inequalities. Models used in APC studies in Korea were limited to the constrained linear models [1-3] or intrinsic estimators (IE), which will be introduced later [4-8]. In this study, we (1) introduce the concept and effects of cohort, (2) briefly describe the recently developed three innovative APC models, and (3) suggest future research direction. Due to space constraint, this study focuses on explaining the concepts and guidelines for empirical applications of the models, rather than providing the detailed algebraic description of each model. The study also focuses on what questions can be addressed and which analytical method should be applied depending on the type of data.
- Concept and effects of (birth) cohort
- A cohort refers to a group of individuals who experience an initial event (e.g., marriage, college entrance) together within a similar period. In medical research, a cohort usually refers to a group recruited as study subjects at the same time point due to their shared clinical characteristics or diseases. In social science including demography or gerontology, a cohort means a birth cohort, a group of individuals born within a specified period. In his classic article [9], Norman Ryder explained that a cohort is defined as people born in a similar time range, entered into the existing social system together, and have similar historical, social, and cultural experiences across life courses. Therefore, cohort effects were generated by the interaction between individuals’ life histories and macro-socioeconomic effects. For example, “the unfortunate class of 1994” in Korea [10] specifically experienced confusions as they were the first generation of the University Scholastic Ability Test and the Academic Divisional System in colleges. As entering the job market during the economic crisis, they also underwent hardships in getting their jobs. Moreover, a more significant portion of the males of the cohort had to serve as active duty soldiers due to the abolition of the Local Soldier System in 1995. Such unfavorable experiences at the critical stages of life would have more considerable adverse effects on their socioeconomic accomplishments throughout their lives, which may bring about distinctive consequences on their health status when comparing to other cohorts.
- Age and period effects
- Cohort analysis aims to estimate the effects of cohort on the outcome of interest. It is also called APC analysis [11] because age and period effects should be considered when estimating cohort effects. To date, APC analysis has been widely used to better understand common interests of demographic and epidemiological research, such as morbidity, mortality, and aging. Age effects for epidemiological studies refer to variations caused by the accumulation of age-related or lifecycle-related exposure, a genetic manifestation of diseases, or physiological changes due to natural physical deterioration [12,13]. Period effects are variations in the time periods that affect all population in society regardless of age and cohort at the same time [12], which may reflect the influence of historical events, such as war, labor market situation, macro-economic changes, infectious disease outbreaks, and medical technology development.
- Each of these three time-related factors has conceptually independent pathway to affect individuals’ health status or health inequalities in society. Therefore, to understand the long-term changes, it is essential to estimate the independent effects of the three factors simultaneously by using the APC analysis.
INTRODUCTION
- Since the concept of the cohort has established, researchers have actively explored statistical methodologies to estimate cohort effects. It is a conundrum of APC analysis that the conventional linear regression model fails to discern cohort effects due to the perfect linear-dependent relationship (cohort = period-age) of the three time-related variables. It is also known as “identification (ID) problem.”
- Researchers have suggested various analytic methods to solve the ID problem. Two methodologies emerged in the 1970s to 1980s were nonlinear models [14] and constrained generalized linear models [15]. The nonlinear models treat at least one of age, period, and cohort as continuous variables, which is then incorporated into the regression model as quadric, cubic, or higher order functions [16]. Setting one or more variables to have a nonlinear relationship with a dependent variable breaks the perfect linear relationship, and enables to estimate the coefficients of the three time variables. Constrained generalized linear models address the ID problem by having an equality constrain, which is derived from an assumption that effects of two adjacent groups of ages, periods, or cohorts are the same.
- Although these two methodologies allowed to estimate coefficient vectors of age, period, and cohort, both methodologies have one crucial limitation: to determine a functional form in a nonlinear model or an equality constraint in a constrained linear model, a researcher should rely on a robust theory or a priori knowledge. That means, it is impossible to estimate the coefficients when such a justification is unavailable. Moreover, as estimates are likely to be sensitive to the selection of the functional form or constraint, a researcher should not arbitrarily select them in any case [17].
- Due to the limitations of the previous models, alternative methodologies to address the ID problem have been suggested. In the past decade, a new class of methodologies in the APC analysis that suggest innovative ways to address the ID problem was developed by Yang, Land, and Fu. They argued that the ID problem is a model-specific issue, rather than a data-specific one, and previous models had to deal with the ID problem as they were based on conventional linear regression models. They suggested APC analysis using IE [18]; and the cross-classified random effect model (CCREM) that applies a multi-level analytic framework [19] and the hierarchical APC (HAPC)-growth curve model. These models have been used widely in various academic areas [20-22].
IDENTIFICATION PROBLEM AND HISTORICAL EVOLUTION OF AGE-PERIOD-COHORT ANALYSIS
- The IE-APC analysis regresses the outcome variable in the nonnull subspace by removing the null space to address the ID problem. The IE-APC analysis employs principal component regression (PCR) techniques. For intuitive interpretation of the coefficients estimated by the PCR using the original scale of A, P, and C, IE-APC transfers them back to the original space (readers can benefit from previous literature for details [12,18]).
- To better understand the IE-APC analysis, we provide an example of an IE-APC study on thyroid cancer incidence in Korea [23]. Since 1999, the incidence of thyroid cancer rapidly increased in Korea [24], which reached the highest level worldwide [25]. However, the cause of the sudden increase of the thyroid cancer incidence was unclear whether it is due to over-diagnosis along with medical detection technologies or an increase in exposure to other factors, such as ionizing radiation or obesity. In this case, APC analysis may provide a hint of the cause of increased cancer incidence. The result of the IE-APC analysis using 5-year age, period, and cohort thyroid cancer incidence at the population level from 1997 to 2011 was presented in Figure 1 [23]. In males, cohort effects showed a U-shape from those who were born in 1932 to those who were born in 1977; however, no significant changes were observed when compared with period effects. In females, relative risks had no significant changes in those who were born in 1932 and 1977, approaching 1. On the other hand, period effects rapidly increased in both males and females from 1997 to 2011. Subsequently, period effects were significantly associated on the elevation of thyroid cancer incidence in Korea, which suggests that its increase may be not due to changes in external environmental factors or obesity rate, but mostly higher detection rate using ultrasound examinations.
- Note that parameter estimators are not always identical with unbiased estimators in IE-APC analysis. Nevertheless, IE-APC has statistically advantageous properties. First, it calculates estimators with better statistical efficiency than previous conventional APC analyses such as constrained generalized linear models [18]. Second, it calculates robust estimators without imposing an additional constraint. Therefore, even when the external information or theory is not established, the model is still estimable [26].
AGE-PERIOD-COHORT ANALYSIS USING AN INTRINSIC ESTIMATOR
- The models above identified the effects of each A, P, and C based on tabular age by period data at population-level. However, the IE-APC analysis presumes the causes of period and cohort effects; however, an empirical analysis on a specific period or cohort characteristics that contributing the trends cannot be performed. Whereas, the HAPC model allows to have additional covariates of period or cohort characteristics in the model to examine specific causes of long-term health status and inequalities [16,19].
- CCREMs are used when two or higher levels have no mutual hierarchical attributes. When CCREMs are applied to APC analysis, effects of age and other individual-level variables are set as fixed effects at level 1, whereas period and cohort effects are set as random effects at level 2 [16,19]. Thus, HAPC analysis can measure random variances of period and cohort effects that were unmeasured at the individual level and can also explain the effects of the period or cohort characteristic variables on trends and changes in the health status and health inequalities [27].
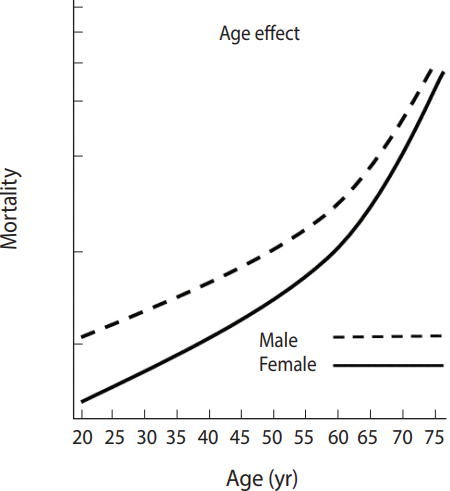
- For a better understanding, an exemplar is provided as follows. A researcher identified long-term trends in adult mortality rates based on data collected in a country and then had the following research questions: (1) How did age, period, and cohort effects vary in contributing to the trend of adult mortality rates? (2) Were cohort characteristics, the number of the population born in a similar period (cohort size) and an economic condition at birth, associated with mortality risks? (3) How different are trajectories of mortality rates between males and females as they aged?
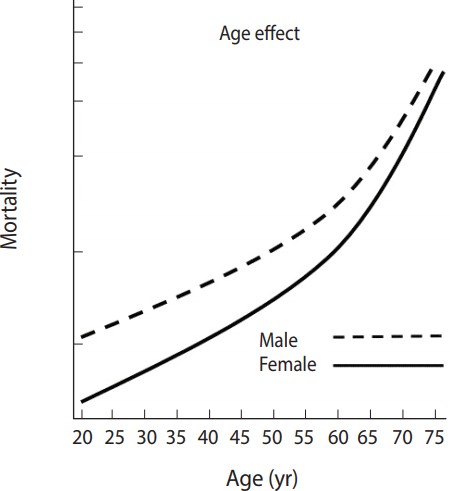
- Figure 2 shows age, period, and cohort effects on the mortality between males and females regarding predicted probabilities of mortality. The effect of one factor is mean values when hold effects of the other two factors at their mean values. In other words, age effects at the far left indicate mortality risks at each age group when period and cohort effects were set to their mean values. The graph of age effects shows that the mortality risk exponentially increased with age. When viewed by cohorts, those who were born in the 1970s had the highest mortality risk among all cohorts, and the cohort effects gradually decreased after that. Mortality risk by period effects decreased over time.
- For the second research question, both an economic indicator variable of birth years and the cohort size variable linked to the birth year variable were included in the model. In Table 1, the variance of random effects in the first model was 0.345. When the two variables were included in the model, increased mortality risk was significantly associated with the two cohort characteristics. A better economic condition at birth was significantly associated with lower mortality risk later. However, a larger cohort size was significantly associated with increased mortality risk. Economic conditions at birth and cohort sizes explained 60.3% [(0.345-0.137)/ 0.345)*100] and 36.2% [(0.345-0.220)/0.345)*100] of cohort variance, respectively.
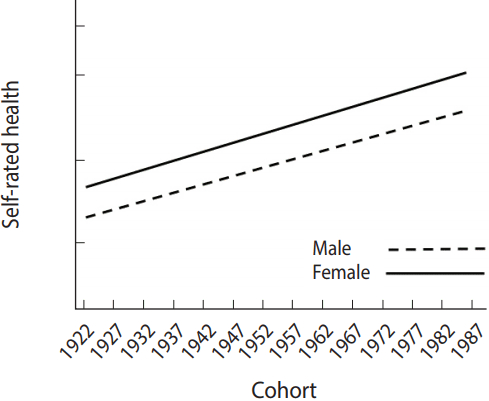
- For the answer to the third research question, Figure 3 shows the results after adding the interaction variables between age and sex to the original model. It shows that the trajectories of mortality risk by ages were different depending on sex, indicating that while males had higher mortality risks in all age groups than females, the difference declines with age.
- As shown, studies using the HAPC model is capable of considering long-term changes in population composition and in social contexts that determine health status and health inequalities; moreover, it can help reveal the specific determinants of the compositional and contextual effects.
HIERARCHICAL AGE-PERIOD-COHORT ANALYSIS USING CROSS-CLASSIFIED RANDOM EFFECT MODELS
- A growth curve model is used to find intra-cohort and inter-cohort variations in health status with age, which shed light on the mechanism for health inequalities throughout the life cycle. This model can answer the following research questions regarding independent age and cohort effects. First, are there any inter-cohort variations in health trajectories during aging process? In other words, are there cohort differences in age trajectories of health? If yes, the variations by age in the previous aging studies without considering cohort effects can be due to confounding factors between age and cohort effects. Second, are there intra-cohort variations in health trajectories during aging process? This question asks whether age trajectories are different depending on socioeconomic status within each cohort. The first question considers a cohort as a homogeneous group, whereas the second question tries to identify further within-cohort heterogeneity. Third, are there inter-cohort variations within intra-cohort variations in health by age and socioeconomic status? This question aimed to identify intra-cohort and inter-cohort heterogeneities revealing how individuals’ aging has changed according to social, historical, and epidemiologic contexts.
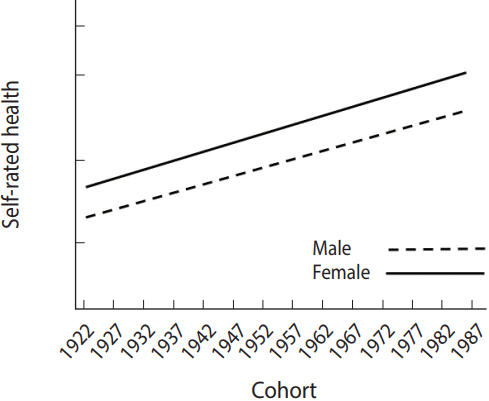
- For a better understanding, an example of the modeling is discussed in Figure 4. The results showed that the mean value of subjective health status increased as cohorts became newer, supporting the hypothesis of inter-cohort variations. In response to the second research question, these results support the hypothesis of intra-cohort inequalities, which demonstrated that continuous inequalities were observed in subjective health status between males and females within cohorts.
- Figure 5 presents an answer to the third research question. To determine whether intra-cohort variations in subjective health by income status are also present between cohorts, a three-way interaction analysis between age, cohort, and income was performed. Figure 5 also shows that changes in inter-cohort differences in subjective health trajectories by income status were altered depending on age. It concluded that growth rates of subjective health by income status were different by cohorts, and the difference got greater.
- The limitation of this model is that period effects are not specified. First, this was because a longitudinal study, unlike synthetic cohort data accumulated for a relatively long time, has insufficient study periods. Thus, period effects are considered negligible or omitted for analysis in studies especially for the elderly. Second, this was due to the impossibility of distinguishing period effects in the accelerated longitudinal panel data. In a growth curve model, level 1 analysis can include age or period depending on a research question; however, age and period are the same for an individual, so that the two aspects cannot be considered simultaneously.
- Along with accumulation of high-quality data and advancement of analytical models, APC methodologies have been being developed to address the ID problem in more innovative ways. Meanwhile, as some researchers report inconsistent estimates of the APC methodologies, the debate on whether the ID problem can be solved or not is still ongoing. As most scholars agree that there is no “magic bullet” model in the APC analyses due to the ID problem, the methodologies presented above should also be carefully applied with a sufficient understanding on the given data and models.
HIERARCHICAL AGE-PERIOD-COHORT-GROWTH CURVE MODEL USING ACCELERATED LONGITUDINAL PANEL DATA
- Mannheim [28] claimed that if a society experiences rapid changes, generation gaps will become wide because differences in inter-cohort historical and cultural experiences are substantial. In analytical perspectives, such societies may have a more significant deviation in cohort effects than other societies. Korea underwent short-term but intense socioeconomic changes after the liberation from the Japanese occupation during the World War II. Thus, APC studies will reveal how distinct are the trajectories of Korean aging, how period and cohort effects have been changed, and what are the biological, historical, and socio-structural factors that contribute to health status and inequalities throughout the life cycle of the Korean population.
- Several national-level health data in Korea are available for the APC methodologies. Data for an IE-APC analysis on incidence or mortality rates due to chronic diseases, including cancers can be obtained from the Korean Statistical Information Service (https://kosis.kr). The HAPC-CCREM analysis can be applied to representative repeated cross-sectional data such as the Korea National Health and Nutrition Examination Survey (started in 1998) and the Community Health Survey (started in 2008). For an HAPC-growth curve analysis, data are available from the Korean Welfare Panel (started in 2006), the Korea Health Panel (started in 2008), and the Korean Longitudinal Study of Ageing (started in 2006), as well as large-scale database provided by the National Health Insurance Service and the Health Insurance Review & Assessment Service. By utilizing the APC analyses, researchers can analyze long-term trends of health status, health behaviors, health inequalities, aging, chronic diseases, and life cycle.
- Furthermore, social and health policies should be specified for dimensions of not only period or age but also cohort. For example, policies may be required based on the cohort size to predict service demands of education, healthcare, and welfare areas to allocate resources. Cohort-specific policies, such as additional childbirth and rearing supports in the early life cycle during economic recessions, may be useful.
CONCLUSION: FUTURE OF AGE-PERIOD-COHORT STUDY IN KOREA
SUPPLEMENTARY MATERIAL
Figure 1. Intrinsic estimator- age-period-cohort analysis of thyroid cancer in Korean adult males (A, B) and females (C, D). From Oh C, et al. Cancer Res Treat 2015;47:362-369 [23].


Figure 2.Example of hierarchical age-period-cohort analysis results on adult mortality rate trends (A: age effect, B: cohort effect).

Figure 5.Differences in age growth trajectory of self-reported health by cohort between income groups.
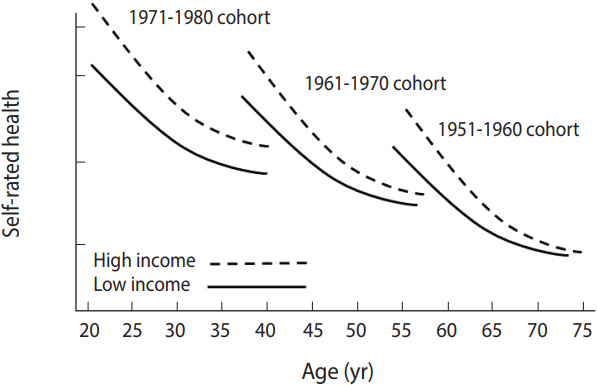

Table 1.Estimates and variances of cohort-specific variables
| β | Variance | |
|---|---|---|
| Covariate adjusted | - | 0.345 |
| GDP at birth | -0.458*** | 0.137 |
| Cohort size | 0.598*** | 0.22 |
- 1. Kwon JW, Song YM, Park HS, Sung J, Kim H, Cho SI. Effects of age, time period, and birth cohort on the prevalence of diabetes and obesity in Korean men. Diabetes Care 2008;31:255-260.ArticlePubMed
- 2. Jhun HJ, Kim H, Cho SI. Time trend and age-period-cohort effects on acute myocardial infarction mortality in Korean adults from 1988 to 2007. J Korean Med Sci 2011;26:637-641.ArticlePubMedPMC
- 3. Choi Y, Kim Y, Park SK, Shin HR, Yoo KY. Age-period-cohort analysis of female breast cancer mortality in Korea. Breast Cancer 2006;13:266-271.ArticlePubMed
- 4. Lee JY, Kim SH. Suicide in South Korea-age-period-cohort analysis, 1983-2003. Korean J Sociol 2010;44:63-94 (Korean).
- 5. Lee HA, Park H. Trends in ischemic heart disease mortality in Korea, 1985-2009: an age-period-cohort analysis. J Prev Med Public Health 2012;45:323-328.ArticlePubMedPMCPDF
- 6. Park C, Jee YH, Jung KJ. Age-period-cohort analysis of the suicide rate in Korea. J Affect Disord 2016;194:16-20.ArticlePubMed
- 7. Seo JY, Choi S, Choi B, Ki M. Age-period-cohort analysis of hepatitis A incidence rates in Korea from 2002 to 2012. Epidemiol Health 2016;38:e2016040.ArticlePubMedPMCPDF
- 8. Jee YH, Cho SI. Age-period-cohort analysis of smoking prevalence among young adults in Korea. Epidemiol Health 2016;38:e2016010.ArticlePubMedPMCPDF
- 9. Ryder NB. The cohort as a concept in the study of social change. Am Sociol Rev 1965;30:843-861.ArticlePubMed
- 10. Weekly Dong-A. Disable students of admission year 1994. Weekly Dong-A; 2000 Dec 14. Seoul: Weekly Dong-A; 2000. p 48-49 (Korean).
- 11. Glenn ND. Cohort analysis. Beverly Hills: Sage; 2005. p 2.
- 12. Yang Y, Land KC. Age-period-cohort analysis : new models, methods, and empirical applications. Boca Raton: CRC Press; 2013. p 1.
- 13. Yang Y. Is old age depressing? Growth trajectories and cohort variations in late-life depression. J Health Soc Behav 2007;48:16-32.ArticlePubMed
- 14. Mason WM, Fienberg SE. Cohort analysis in social research: beyond the identification problem. New York: Springer; 1985. p 1-8.
- 15. Mason KO, Mason WM, Winsborough HH, Poole WK. Some methodological issues in cohort analysis of archival data. Am Sociol Rev 1973;38:242-258.Article
- 16. Yang Y, Land KC. A mixed models approach to the age-periodcohort analysis of repeated cross-section surveys, with an application to data on trends in verbal test scores. Sociol Methodol 2006;36:75-97.Article
- 17. Reither EN, Masters RK, Yang YC, Powers DA, Zheng H, Land KC. Should age-period-cohort studies return to the methodologies of the 1970s? Soc Sci Med 2015;128:356-365.ArticlePubMedPMC
- 18. Yang Y, Schulhofer-Wohl S, Fu WJ, Land KC. The intrinsic estimator for age-period-cohort analysis: what it is and how to use it. Am J Sociol 2008;113:1697-1736.Article
- 19. Yang Y, Land KC. Age–period–cohort analysis of repeated cross-section surveys: fixed or random effects? Sociol Methods Res 2008;36:297-326.Article
- 20. Dassonneville R. Questioning generational replacement. An age, period and cohort analysis of electoral volatility in the Netherlands, 1971–2010. Elect Stud 2013;32:37-47.Article
- 21. Jeon SY, Reither EN, Masters RK. A population-based analysis of increasing rates of suicide mortality in Japan and South Korea, 1985-2010. BMC Public Health 2016;16:356.ArticlePubMedPMC
- 22. Reither EN, Hauser RM, Yang Y. Do birth cohorts matter? Ageperiod-cohort analyses of the obesity epidemic in the United States. Soc Sci Med 2009;69:1439-1448.ArticlePubMedPMC
- 23. Oh CM, Jung KW, Won YJ, Shin A, Kong HJ, Lee JS. Age-periodcohort analysis of thyroid cancer incidence in Korea. Cancer Res Treat 2015;47:362-369.ArticlePubMedPDF
- 24. Oh CM, Won YJ, Jung KW, Kong HJ, Cho H, Lee JK, et al. Cancer statistics in Korea: incidence, mortality, survival, and prevalence in 2013. Cancer Res Treat 2016;48:436-450.ArticlePubMedPMCPDF
- 25. Ferlay J, Soerjomataram I, Dikshit R, Eser S, Mathers C, Rebelo M, et al. Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 2015;136:E359-E386.ArticlePubMed
- 26. Land KC, Zang E, Fu Q, Guo X, Jeon SY, Reither EN. Playing with the rules and making misleading statements: a response to Luo, Hodges, Winship, and Powers. Am J Sociol 2016;122:962-973.Article
- 27. Yang Y. Aging, cohorts, and methods. In: George LK, Ferraro KF, Carr DS, Wilmoth JM, Wolf D, eds. Handbook of aging and the social sciences. Amsterdam: Elsevier; 2011. p 17-30.
- 28. Mannheim K. Essays on the sociology of knowledge. [cited 2017 Dec 10]. Available from: https://archive.org/stream/essaysonsociolog00mann/essaysonsociolog00mann_djvu.txt.Article
REFERENCES
Figure & Data
References
Citations
Citations to this article as recorded by 

- Environmental asbestos exposure from nephrite jade mining and lung cancer
Hsiao-Yu Yang, Sugio Furuya, Naoki Toyama
Journal of the Formosan Medical Association.2024; 123(7): 796. CrossRef - 성인 음주행동 변화의 연령-기간-코호트 분석
광기 김, 정 제갈, 민주 최, 은실 전, 희원 강, 지희 김, 선혜 최, 경원 오
Public Health Weekly Report.2024; 17(21): 877. CrossRef - Descriptive Analysis of Gastric Cancer Mortality in Korea, 2000-2020
Tung Hoang, Hyeongtaek Woo, Sooyoung Cho, Jeeyoo Lee, Sayada Zartasha Kazmi, Aesun Shin
Cancer Research and Treatment.2023; 55(2): 603. CrossRef - Vehicle ownership rates: The role of lifecycle, period, and cohort effects
Julene Paul, Evelyn Blumenberg
Transportation Research Interdisciplinary Perspectives.2023; 21: 100892. CrossRef - Finding Gaps of Net Worth between Generations in 2012-2021 Using Survey Data of Household Finances and Living Conditions : Using Age-Period-Cohort Analysis focusing on SMA and Non-SMA
Haekyung Park, Seungun Han, Sang-Il Kim
Journal of Korea Planning Association.2023; 58(3): 167. CrossRef - Secular trends in the incidence of major depressive disorder and dysthymia in China from 1990 to 2019
Ming Li, Wenlong Gao, Yuqi Zhang, Qiuxia Luo, Yuanyuan Xiang, Kai Bao, Noha Zaki
BMC Public Health.2023;[Epub] CrossRef - Decrease in household secondhand smoking among South Korean adolescents associated with smoke-free policies: grade-period-cohort and interrupted time series analyses
Hana Kim, Heewon Kang, Sung-il Cho
Epidemiology and Health.2023; : e2024009. CrossRef - Representative Sampling of the Via Assessment Suite for Adults
Robert E. McGrath, Mitch Brown, Bina Westrich, Hyemin Han
Journal of Personality Assessment.2022; 104(3): 380. CrossRef - Physical Performance in Older Cohorts: A Comparison of 81-Year-Old Swedish Men and Women Born Twelve Years Apart—Results from the Swedish Study “Good Aging in Skåne”
Henrik Ekström, Sölve Elmståhl, Lena Sandin Wranker, Hélio J. Coelho-Júnior
Journal of Aging Research.2021; 2021: 1. CrossRef - Recent increase in pertussis incidence in Korea: an age-period-cohort analysis
Chanhee Kim, Seonju Yi, Sung-il Cho
Epidemiology and Health.2021; 43: e2021053. CrossRef - Sepsis in the new millennium – Are we improving?
Graeme J. Duke, John L. Moran, John D. Santamaria, David V. Pilcher
Journal of Critical Care.2020; 56: 273. CrossRef - Time Trends for Prostate Cancer Incidence from 2003 to 2013 in South Korea: An Age-Period-Cohort Analysis
Hyun Young Lee, Do Kyoung Kim, Seung Whan Doo, Won Jae Yang, Yun Seob Song, Bora Lee, Jae Heon Kim
Cancer Research and Treatment.2020; 52(1): 301. CrossRef - Latent tuberculosis infection screening and treatment in congregate settings (TB FREE COREA): protocol for a prospective observational study in Korea
Jinsoo Min, Hyung Woo Kim, Helen R Stagg, Marc Lipman, Molebogeng X Rangaka, Jun-Pyo Myong, Hyeon Woo Yim, Jeong Uk Lim, Yunhee Lee, Hyeon-Kyoung Koo, Sung-Soon Lee, Jae Seuk Park, Kyung Sook Cho, Ju Sang Kim
BMJ Open.2020; 10(2): e034098. CrossRef - Age-stratified anti-tuberculosis drug resistance profiles in South Korea: a multicenter retrospective study
Eung Gu Lee, Jinsoo Min, Ji Young Kang, Sung Kyoung Kim, Jin Woo Kim, Yong Hyun Kim, Hyoung Kyu Yoon, Sang Haak Lee, Hyung Woo Kim, Ju Sang Kim
BMC Infectious Diseases.2020;[Epub] CrossRef - Community context, birth cohorts and childhood body mass index trajectories: Evidence from the China nutrition and health survey 1991–2011
Jing Liang, Fang Tang, Junfeng Jiang, Hai Zhang, Mohammedhamid Osman, Bhawana Shrestha, Peigang Wang
Health & Place.2020; 66: 102455. CrossRef - Relationship between incidence and prevalence in psychotic disorders: An incidence–prevalence–mortality model
Baptiste Pignon, Franck Schürhoff, Grégoire Baudin, Andrea Tortelli, Aziz Ferchiou, Ghassen Saba, Jean‐Romain Richard, Antoine Pelissolo, Marion Leboyer, Andrei Szöke
International Journal of Methods in Psychiatric Research.2018;[Epub] CrossRef

 KSE
KSE
 PubReader
PubReader ePub Link
ePub Link Cite
Cite