Articles
- Page Path
- HOME > Epidemiol Health > Volume 39; 2017 > Article
-
Original Article
The association between smoking or passive smoking and cardiovascular diseases using a Bayesian hierarchical model: based on the 2008-2013 Korea Community Health Survey -
Whanhee Lee
 , Sung-Hee Hwang
, Sung-Hee Hwang , Hayoung Choi
, Hayoung Choi , Ho Kim
, Ho Kim
-
Epidemiol Health 2017;39:e2017026.
DOI: https://doi.org/10.4178/epih.e2017026
Published online: June 22, 2017
Graduate School of Public Health, Seoul National University, Seoul, Korea
- Correspondence: Ho Kim Graduated School of Public Health, Seoul National University, 1 Gwanak-ro, Gwanak-gu, Seoul 08826, Korea E-mail: hokim@snu.ac.kr
• Received: January 2, 2017 • Accepted: January 17, 2017
©2017, Korean Society of Epidemiology
This is an open-access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
-
OBJECTIVES
- Smoking and passive smoking have been extensively reported as risk factors of cardiovascular morbidity and mortality. Despite the biological mechanisms underlying the impact of hazardous chemical substances contained in tobacco in cardiovascular diseases (CVD), studies investigating the association between smoking and passive smoking with morbidity are at an inchoate stage in Korea. Therefore, this study aimed to estimate the risks of smoking and passive smoking on cardiovascular morbidity at the national and regional levels.
-
METHODS
- This study calculated sex-standardized and age-standardized prevalence of CVD and smoking indices in 253 community health centers (si/gun/gu) in Korea using the 2008-2013 Korea Community Health Survey data. Furthermore, a Bayesian hierarchical model was used to estimate the association of smoking and passive smoking with the prevalence of CVD from the national and regional community health centers.
-
RESULTS
- At the national level, smoking was significantly associated with stroke (relative risk [RR], 1.060) and hypertension (RR, 1.016) prevalence, whilst passive smoking at home and work were also significantly associated with prevalence of stroke (RR, 1.037/1.013), angina (RR, 1.016/1.006), and hypertension (RR, 1.010/1.004). Furthermore, the effects of smoking and passive smoking were greater in urban-industrial areas than in rural areas.
-
CONCLUSIONS
- The findings of this study would provide grounds for national policies that limit smoking and passive smoking, as well as regionally serve as the basis for region-specific healthcare policies in populations with high CVD vulnerability.
- Smoking and passive smoking have extensively been documented as risk factors of morbidity and mortality by a number of diseases [1-4]. Among more than 4,000 types of chemical substances contained in a cigarette, polycyclic aromatic hydrocarbons and oxidizing gases cause cardiac toxicity [1], having adverse effects on various cardiovascular diseases (CVD), including coronary artery disease, ischemic stroke, non-traumatic subarachnoid hemorrhage [5,6].
- The World Health Organization reported that CVD-related death (1.69 million) is the leading cause of smoking-related death. In a study on 360 thousand US men, smoking has been identified as a key risk factor for lung cancer, chronic heart disease, and stroke [3]. In addition, a Norwegian study revealed that smokers are 2.74 times more likely to have a stroke and 6.74 times more likely to die from it than are non-smokers [4]. Similar to the effects of smoking, passive smoking has also been reported to be the cause of respiratory and CVD, various cancers, and premature deaths in non-smoking adults [7]. Other studies have suggested that secondhand smoking in non-smokers increases their risk of developing a heart disease by 25 to 30% [8-10].
- In South Korea (hereafter Korea), several studies have reported that smoking increases the risk of CVD-related death in adults [11-13]. As of 2012, the number of smoking-related deaths was 4,148 for stroke and 3,858 for ischemic heart disease, which are ranked the second and third highest causes of death by an illness respectively [14]. Furthermore, it also has been reported that 26.7% of all CVD-related deaths in men and women adults in Korea are caused by smoking [13]. Although adult smoking rate in Korea has consistently been on a decline since 1998 [15], past smoking history may have an impact on death [11]. Moreover, medical expenses and patient population related to hypertension, heart disease, and cerebrovascular disease are continuously on the rise [16], suggesting that smoking is a health hazard in terms of CVD and mortality requiring much attention.
- As shown here, though there have been much research investigating the association between smoking and death by CVD in Korea, studies on smoking and morbidity is relatively lacking. Hence, this study aimed at quantitatively analyzing the association between smoking and the prevalence of various CVD (i.e., hypertension, stroke, myocardial infarction, angina), and to evaluate the relative risk (RR) of smoking on the prevalence of CVD using data from a large-scale cross-sectional study with more than 1.5 million participants. We also examined the effects of passive smoking on the prevalence of CVD.
INTRODUCTION
- Data
- Data from the 2008-2013 Korea Community Health Survey (KCHS) involving 253 community health centers were used for this study [17]. The KCHS was conducted by the Korea Centers for Disease Control and Prevention, and data collected from adults aged 19 years or older via interviews. The sample was extracted from an average of 900 adults per community (si/gun/gu) based on the type of housing within each dong/eup/myeon. The primary sample region was obtained using a probability proportional to size systematic sampling, after which the secondary sample families were selected [18]. A total of 1,567,930 people were included in the KCHS data used in this study (2008: 200,800; 2009: 220,258; 2010: 230,712; 2011: 229,229; 2012: 229,226; 2013: 228,781), and the participants were randomly extracted every year. Using this data, we calculated the prevalence of 4 CVD (hypertension in adults ≥ 30 years, stroke in adults ≥ 50 years, myocardial infarction in adults ≥ 40 years, angina in adults ≥ 40 years), smoking-related regional parameters (current smoking rate, passive smoking rate at home, and passive smoking rate at work), body mass index (BMI), and monthly drinking rate by community (si/gun/gu), after reflecting gender/age distributions based on the year of study. The prevalence of CVD was measured, based on a self-reported response regarding a physician’s diagnosis, whilst BMI and monthly drinking rates were also measured with self-reported data.
- Statistical analysis
- A generalized linear mixed model (GLMM) was used to analyze the association among regional and national smoking indices and prevalence of CVD that were repeatedly measured from 2008-2013. The prevalence of 4 CVD (hypertension in adults ≥ 30 years, stroke in adults ≥ 50 years, myocardial infarction in adults ≥ 40 years, and angina in adults ≥ 40 years) was set as the response variables. A Shapiro-Wilk test revealed that the prevalence of all 4 diseases did not follow a normal distribution, but instead showed a gamma distribution. Hence, a GLMM that assumes gamma distribution for the response variables was used. A log function was used as the link function. Mean BMI and monthly drinking rate per community (si/gun/gu) for 2008-2013, were set as the respective confounding variables and covariate, and a linear adjustment was made for annual effects to consider the effects of time. Smoking indices (current smoking rate, passive smoking rate at home, passive smoking rate at work) were used as the response variables, and we predicted associations with response variables with equal confounding variables and covariates.
- Furthermore, a Bayesian hierarchical model was used with a GLMM to measure the effects of smoking indices of each community (si/gun/gu) and adjust for the correlations according to distance. The associations between community (si/gun/gu)-specific smoking indices and CVD were examined with random intercept and random slope, and the prior distributions of random intercept and random slope were assumed to follow a normal distribution with mean zero and an assumption that the inverse of variance follows a gamma distribution (parameter= 1, 5*10-5). Spatial correlation was adjusted for, with random intercept using the Besag-York-Mollie method [19], and all random intercepts and random slopes were assumed to be independent. Based on existing studies, the prior distribution of fixed effects was assumed a multivariate normal, which assumes variance to be a Gaussian Markov random field [20], and the posterior credibility interval (CI) was estimated based on the prior distribution. All analyses were performed using the R and R version 3.2.2 (https://cran.r-project.org/bin/windows/base/old/3.2.2/) for integrated nested Laplace approximation (INLA) [21]. More detailed formula and prior conditions are reported in Appendix 1.
MATERIALS AND METHODS
- Table 1 shows the descriptive statistics for the variables used in this study. Hypertension over 30 years was the most prevalent (18.2%) throughout the 6 years of study (2008-2013), while angina over 40 years was the least prevalent (1.9%). The distributions of prevalence varied widely across the country. The average smoking rate as an interest variable during 6 years was 25.2% (14.9 to 33.4%), with an average passive smoking rate at home of 11.8% (2.3 to 37.3%) and an average passive smoking rate at work of 29.2% (6.0 to 76.7%).
- Table 2 shows the top and bottom 5 community health centers in terms of the prevalence of CVD and smoking indices (6-year average). Hypertension over 30 years was generally prevalent in the Gangwon province (21.72 to 22.35%) and less prevalent in community health centers in the Gyeongsang province and Jeolla province (14.03 to 14.72%). Stroke over 50 years was generally prevalent in community health centers in the North Gyeongsang province (4.68 to 5.33%) and less prevalent in the South Jeolla province (1.93 to 2.12%). Myocardial infarction over 40 years tended to be prevalent in community health centers in Seoul and the Gyeonggi province (2.12 to 2.25%) and less prevalent in community health centers in North Jeolla province (0.78 to 0.83%). Angina over 40 years tended to be prevalent in community health centers in Busan (2.88 to 3.25%) and less prevalent in the North Jeolla province (1.03 to 1.08%). In terms of smoking parameters, smoking rate did not vary by region. Community health centers in Jeju Island showed higher passive smoking rates at home (19.88 to 21.80%) while community health centers in Ulsan showed higher passive smoking rates at work (40.93 to 41.70%).
- The national average RR of smoking indices on the prevalence of CVD is shown in Table 3, whilst the regional average (RR) for top and bottom 5 regions is shown in Table 4. All RR shown in Tables 3 and 4 represent RR when smoking parameters increase by 5%. As shown in Table 3, smoking rate was most highly associated with stroke (RR, 1.060; 95% CI, 1.022 to 1.100), and it was also significantly associated with hypertension (RR, 1.016; 95% CI, 1.004 to 1.029). Passive smoking at home was most strongly associated with a rise in the prevalence of stroke (RR, 1.037; 95% CI, 1.023 to 1.051), and its RR for hypertension, stroke, and angina (but not myocardial infarction) was statistically significant (RR, 1.010 to 1.037). Passive smoking at work had the greatest effect on stroke (RR, 1.013; 95% CI, 1.007 to 1.019) and also had a significant effect on hypertension (RR, 1.004; 95% CI, 1.002 to 1.006).
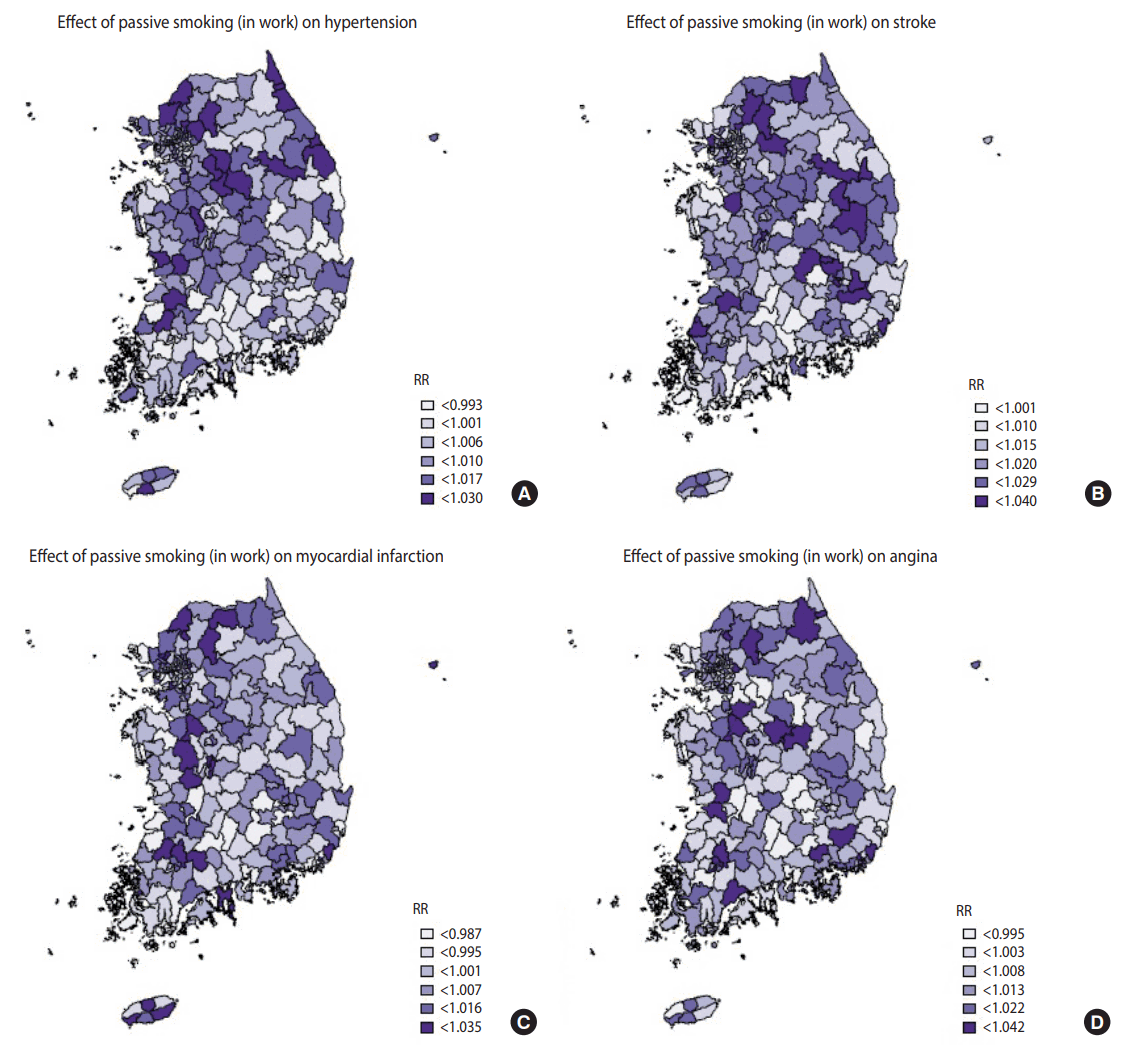
- Table 4 shows the top and bottom three community health centers in terms of the RRs of smoking indices, whilst Figures 1-3 are national maps showing the effects of community-specific smoking rate and passive smoking rate at home and work on the prevalence of CVD. RR of smoking rate for hypertension was high in community health centers in Gyeonggi and Gangwon provinces (RR, 1.042 to 1.046) and low in community health centers in North Jeolla and Gyeonsang provinces (RR, 0.985 to 0.996). Furthermore, smoking was strongly associated with stroke in community health centers in North Gyeongsang province (RR, 1.095 to 1.099) but weakly associated with stroke in community health centers in Busan and Ulsan (RR, 1.033 to 1.034). The RR of smoking for myocardial infarction was high in community health centers in Daejeon (RR, 1.029 to 1.029), but there were no regional differences in terms of low RR (RR, 0.973 to 0.983). The effects of smoking on angina was high in the Gyeonggi region (RR, 1.040 to 1.035) and low in the southern region of the Korean peninsula (North Gyeonsang, North Jeolla, and Jeju Island) (RR, 0.975 to 0.989). The distributions of RR of passive smoking at home and work were similar to those of smoking, and the community rankings were similar as well. Exposure to passive smoking at home (RR, 1.003 to 1.037) had greater impact on all 4 CVD than did exposure to passive smoking at work (RR, 0.998 to 1.013). In addition, the RR of all smoking indices tended to be higher in the Seoul metropolitan area (Figures 1-3).
RESULTS
- This study analyzed the associations between regional smoking indices (smoking rate and passive smoking rate at home and work) and 4 CVD (hypertension in adults ≥ 30 years, stroke in adults ≥ 50 years, myocardial infarction in adults ≥ 40 years, angina in adults ≥ 40 years) with the KCHS data using a Bayesian hierarchical model. The results showed that smoking rate was significantly associated with stroke (RR, 1.060) and hypertension (RR, 1.016), and that passive smoking was significantly associated with stroke (RR, 1.013 to 1.037), angina (RR, 1.006 to 1.016), and hypertension (RR, 1.004 to 1.010) at the national level. Furthermore, exposure to passive smoking at home (RR, 1.003 to 1.037) had a greater impact on CVD than did exposure to passive smoking at work (RR, 0.998 to 1.013).
- In addition to the national-level analysis, this study also analyzed the effects of smoking regionally in 253 regions, based on the assumption that specific regional features (geographical location, environment, income, population matrix) may have varying effects on the prevalence of CVD and may alter the effects of smoking on CVD. Our findings showed that RR of smoking varied across regions, suggesting that the effects of smoking on CVD varied across regions. The effects of smoking and passive smoking on all CVD were high in urban-industrial regions.
- Nicotine, the primary ingredient of tobacco, is a sympathetic stimulant that acts on the central and peripheral nervous systems to stimulate the release of catecholamine and other neurotransmitters. It leads to cardiovascular consequences, such as elevating the heart rate, blood pressure, and cardiac output. Furthermore, it leads to a rise in low-density lipoprotein and decrease in high-density lipoprotein by mobilizing free fatty acids, thereby intensifying vasoconstriction and accelerating the progression of blood epithelial cell injury and atherosclerosis [1]. Carbon monoxide that is inhaled through smoking and passive smoking binds with hemoglobin to induce hypoxia, which increases the number of red blood cells and subsequently, blood viscosity thereby, having a direct impact on thrombosis and atherosclerosis [22]. Through these actions, smoking not only causes coronary artery diseases but also induces structural damage to arterial walls, and has also been associated with ischemic stroke caused by atherosclerosis and nontraumatic subarachnoid hemorrhage caused by formation and rupture of aneurysm [23].
- This study presents data that support these biological causes. Although smoking indices were not statistically significantly associated with myocardial infarction and angina, the RR of smoking was above 1 for all CVDs at the national level (RR, 1.004 to 1.010). These results are in line with those reported by US and Norwegian studies on the relationship between smoking and heart diseases [3,4]. According to a foreign 20-year retrospective study, the greater the degree of exposure to passive smoking (cotinine concentration) was, the greater the risk for coronary artery disease and stroke [24]. Another study involving experimental and control groups revealed that the risk for myocardial infarction increases by 68% among passive smokers [25]. Furthermore, a meta-analysis of studies in 6 countries found that the RR for CVDs was between 1.2 and 1.3 [26]. In one study, passive smoking was found to be more of a health-hazard than direct smoking because smoke from the tip of a cigarette is more harmful than filtered smoke [27]. Our study also found similar results, and our results showed that the RR of passive smoking at home on angina (RR, 1.016) was higher than that of direct smoking (RR, 1.007).
- Nevertheless, this study has a few limitations. First, this study merely analyzed associations and not the causal relationships between smoking indices and CVD. It is difficult to consider the temporal relations of smoking indices and CVD with KCHS data because this was a cross-sectional study [18]. In addition, this study did not consider risk factors at the individual level, so the results should be interpreted as a regional association and not as causal relations. Second, we were able to predict regions that were vulnerable to smoking and passive smoking but could not identify the biological and epidemiological causes of their vulnerability. More specifically, this study was able to verify that people with CVD in urban regions (including industrial regions) are relatively more vulnerable to smoking and passive smoking, but we could not shed light on the fundamental hypothesis and cause after adjusting for gender and age. We expect follow-up studies to evaluate the cause and to explain these results via diverse investigations and advanced analytical methods. Finally, this study did not consider social indicators. CVD may be influenced by social factors, such as income level and environment, but this study could not take these into considerations due to a lack of appropriate data. However, we partially compensated for this by examining potential regional features through performing a longitudinal analysis using a random effect model [28,29].
- Despite a few limitations, this study offers several benefits. First, the large sample size of more than 1.5 million subjects increased the accuracy of our analysis in identifying the associations between CVD and smoking indices. Particularly, most of the 4 CVD studied were strongly associated with the smoking indices, with stroke having the greatest association with smoking and passive smoking (RR, 1.013 to 1.060). Second, by using an advanced statistical method, we were able to predict RRs not only at the national but also regional levels. The INLA method [20] predicts post-distributions as does the Markov Chain Monte Carlo method that is widely used in Bayesian statistical analysis, but the INLA is quicker and is easier for expanding distributions [30]. This study is valuable in that it simultaneously analyzed national and regional level risks by performing a Bayesian hierarchical analysis, considering regional correlations with the INLA.
- Furthermore, the findings of this study can be used as the grounds for public healthcare policies that limit smoking and passive smoking nationwide to promote people’s health. Particularly, they will contribute to devising region-specific healthcare policies for regions populated by groups of people who may be vulnerable to CVD. In other words, there is a need to implement more active measures to limit smoking and to respond to the problems of indoor passive smoking in regions with high populations of people vulnerable to CVD, such as the elderly and financially unstable groups.
DISCUSSION
ACKNOWLEDGEMENTS
SUPPLEMENTARY MATERIAL
Figure 1.Geographical distribution of relative risks (RR). The associations between 4 cardiovascular diseases (A) hypertension over 30 years, (B) stoke over 50 years, (C) myocardial infarction over 40 years, and (D) angina over 40 years and smoking.
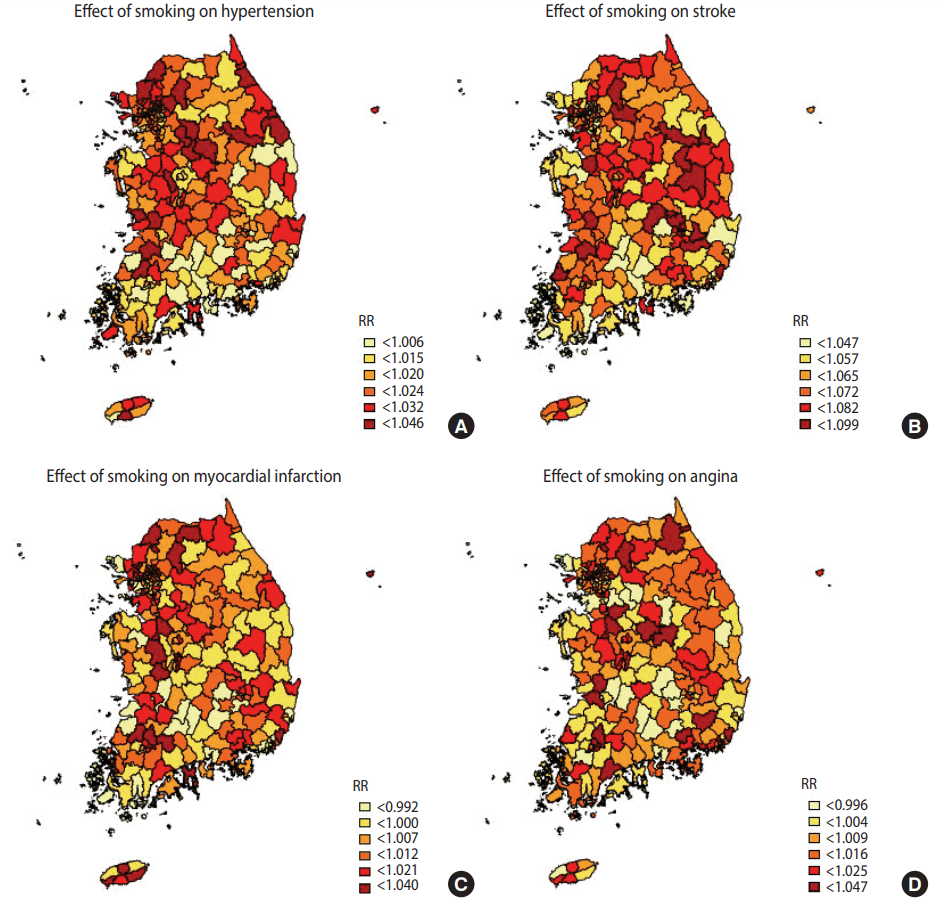

Figure 2.Geographical distribution of relative risks (RR). The associations between 4 cardiovascular diseases (A) hypertension over 30 years, (B) stoke over 50 years, (C) myocardial infarction over 40 years, and (D) angina over 40 years and passive smoking at home.
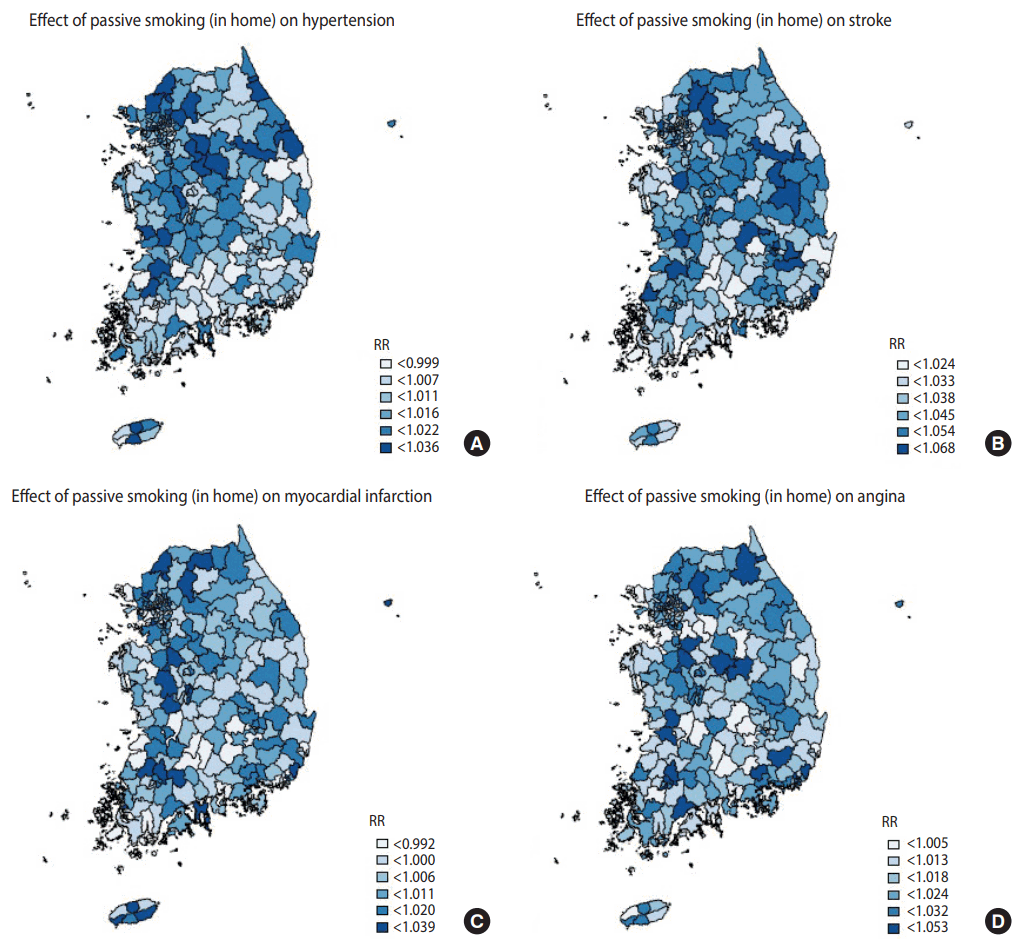

Figure 3.Geographical distribution of relative risks (RR). The associations between 4 cardiovascular diseases (A) hypertension over 30 years, (B) stoke over 50 years, (C) myocardial infarction over 40 years, and (D) angina over 40 years and passive smoking at work.
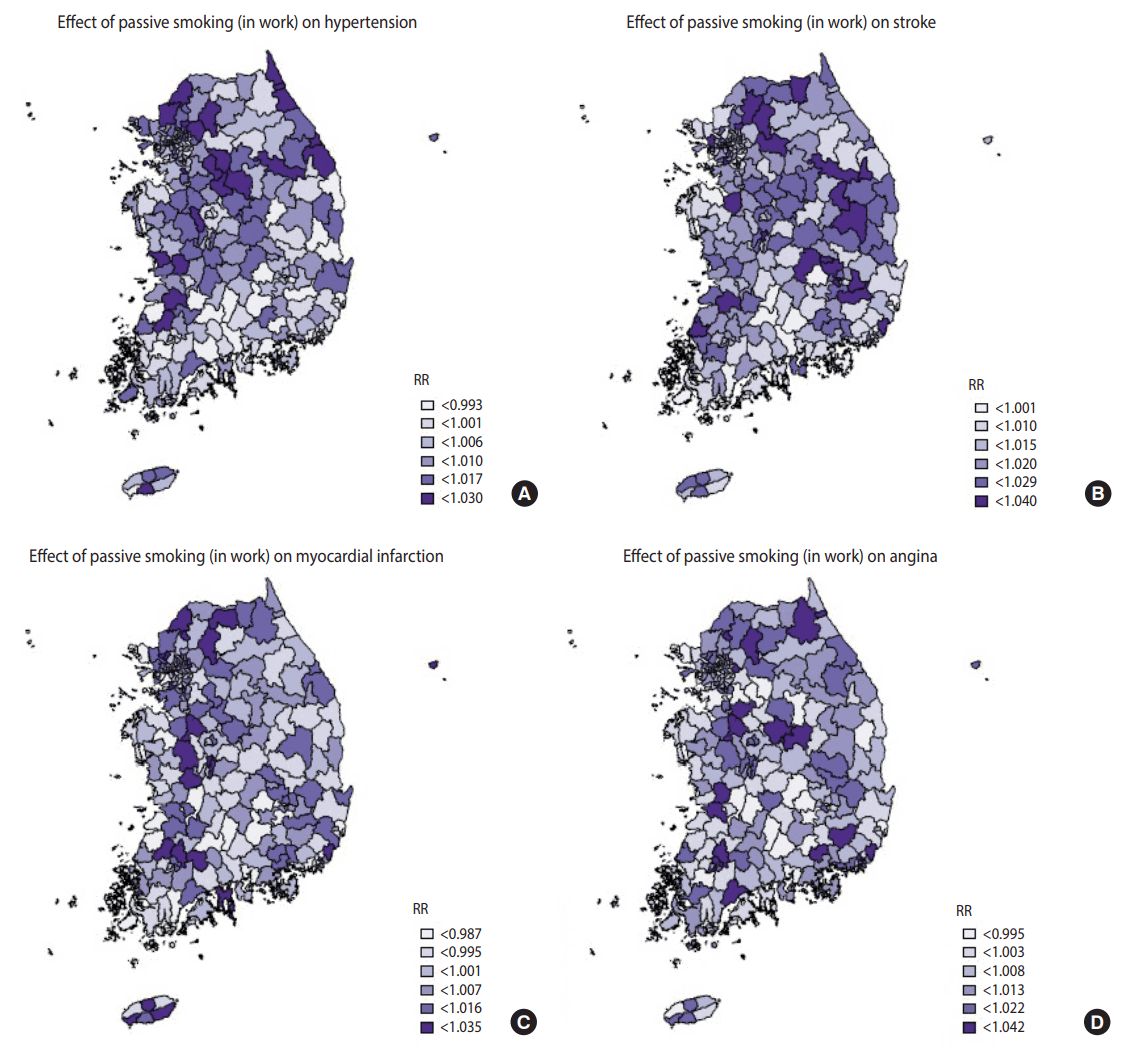

Table 1.Descriptive statistics for regional prevalence of CVD and confounders
Table 2.Higher and lower 5 community health centers (si/gun/gu) of cardiovascular disease prevalence
Table 3.Relative risk of smoking/passive smoking (at home)/passive smoking (at work) by cardiovascular diseases (per 5% smoking or passive smoking rate)
Table 4.Higher and lower 5 community health centers (si/gun/gu) of relative risk (RR) to smoking/passive smoking (at home)/passive smoking (at work)
- 1. Bullen C. Impact of tobacco smoking and smoking cessation on cardiovascular risk and disease. Expert Rev Cardiovasc Ther 2008;6:883-895.ArticlePubMed
- 2. Centers for Disease Control and Prevention (CDC). Smoking-attributable mortality, years of potential life lost, and productivity losses--United States, 2000-2004. MMWR Morb Mortal Wkly Rep 2008;57:1226-1228.ArticlePubMed
- 3. Kuller LH, Ockene JK, Meilahn E, Wentworth DN, Svendsen KH, Neaton JD. Cigarette smoking and mortality. MRFIT Research Group. Prev Med 1991;20:638-654.ArticlePubMed
- 4. Håheim LL, Holme I, Hjermann I, Leren P. Risk factors of stroke incidence and mortality. A 12-year follow-up of the Oslo Study. Stroke 1993;24:1484-1489.ArticlePubMed
- 5. Kannel WB, D’Agostino RB, Belanger AJ. Fibrinogen, cigarette smoking, and risk of cardiovascular disease: insights from the Framingham Study. Am Heart J 1987;113:1006-1010.ArticlePubMed
- 6. Ockene IS, Miller NH. Cigarette smoking, cardiovascular disease, and stroke: a statement for healthcare professionals from the American Heart Association. American Heart Association Task Force on Risk Reduction. Circulation 1997;96:3243-3247.ArticlePubMed
- 7. International Agency for Research on Cancer (IARC). IARC monographs on the evaluation of carcinogenic risks to humans; 2004 [cited 2017 Jun 20]. Available from: http://monographs.iarc.fr/ENG/Monographs/vol106/index.php.
- 8. Glantz SA, Parmley WW. Passive smoking and heart disease. Epidemiology, physiology, and biochemistry. Circulation 1991;83:1-12.ArticlePubMed
- 9. Law MR, Morris JK, Wald NJ. Environmental tobacco smoke exposure and ischaemic heart disease: an evaluation of the evidence. BMJ 1997;315:973-980.ArticlePubMedPMC
- 10. Thun M, Henley J, Apicella L. Epidemiologic studies of fatal and nonfatal cardiovascular disease and ETS exposure from spousal smoking. Environ Health Perspect 1999;107 Suppl 6:841-846.ArticlePubMed
- 11. Lee EH, Park SK, Ko KP, Cho IS, Chang SH, Shin HR, et al. Cigarette smoking and mortality in the Korean Multi-center Cancer Cohort (KMCC) study. J Prev Med Public Health 2010;43:151-158 (Korean).ArticlePubMedPDF
- 12. Meng KH. Smoking-attributable mortality among Korean adults. Korean J Epidemiol 1988;10:138-145 (Korean).
- 13. Jee SH, Lee JK, Kim IS. Smoking-attributable mortality among Korean adults: 1981-2003. Korean J Epidemiol 2006;28:92-99 (Korean).
- 14. Jung KJ, Yun YD, Baek SJ, Jee SH, Kim IS. Smoking-attributable mortality among Korean adults, 2012. J Korea Soc Health Inform Stat 2013;38:36-48 (Korean).
- 15. Korean Statistical Information Service. Current smoking rate 2008-2016. [cited 2017 Jul 20]. Available from: http://kosis.kr/statHtml/statHtml.do?orgId=117&tblId=DT_H_SM&conn_path=I2&language=en.
- 16. Kim J, Son M. National health insurance statistical yearbook. Seoul: Health Insurance Review and Assessment Service and National Health Insurance Service; 2014. p 62-67 (Korean).
- 17. Kim YT, Choi BY, Lee KO, Kim H, Chun JH, Kim SY, et al. Overview of Korean Community Health Survey. J Korean Med Assoc 2012;55:74-83 (Korean).Article
- 18. Lee WH, Choo JY, Son JY, Kim H. Association between long-term exposure to air pollutants and prevalence of cardiovascular disease in 108 South Korean communities in 2008-2010: a cross-sectional study. Sci Total Environ 2016;565:271-278.ArticlePubMed
- 19. Besag J, York J, Mollié A. Bayesian image restoration, with two applications in spatial statistics. Ann Inst Stat Math 1991;43:1-20.Article
- 20. Rue H, Martino S, Chopin N. Approximate Bayesian inference for latent Gaussian models by using integrated nested Laplace approximations. J R Stat Soc Series B Stat Methodol 2009;71:319-392.Article
- 21. Martino S, Rue H. Implementing approximate Bayesian inference using integrated nested Laplace approximation: a manual for the INLA program; 2008 [cited 2017 Jun 20]. Available from: http://www.bias-project.org.uk/GMRFCourse/inla-program.pdf.
- 22. Ambrose JA, Barua RS. The pathophysiology of cigarette smoking and cardiovascular disease: an update. J Am Coll Cardiol 2004;43:1731-1737.ArticlePubMed
- 23. Kurth T, Kase CS, Berger K, Gaziano JM, Cook NR, Buring JE. Smoking and risk of hemorrhagic stroke in women. Stroke 2003;34:2792-2795.ArticlePubMed
- 24. Whincup PH, Gilg JA, Emberson JR, Jarvis MJ, Feyerabend C, Bryant A, et al. Passive smoking and risk of coronary heart disease and stroke: prospective study with cotinine measurement. BMJ 2004;329:200-205.ArticlePubMedPMC
- 25. Wells AJ. Heart disease from passive smoking in the workplace. J Am Coll Cardiol 1998;31:1-9.ArticlePubMed
- 26. He J, Vupputuri S, Allen K, Prerost MR, Hughes J, Whelton PK. Passive smoking and the risk of coronary heart disease--a metaanalysis of epidemiologic studies. N Engl J Med 1999;340:920-926.ArticlePubMed
- 27. Dobson R. Smoke from cigarette tip is more toxic than main inhaled smoke. BMJ 2005;331:1425.ArticlePubMed
- 28. Laird NM, Ware JH. Random-effects models for longitudinal data. Biometrics 1982;38:963-974.ArticlePubMed
- 29. Liang KY, Zeger SL. Longitudinal data analysis using generalized linear models. Biometrika 1986;73:13-22.ArticlePDF
- 30. Blangiardo M, Cameletti M. Spatial and Spatio-temporal Bayesian models with R-INLA. New York: John Wiley & Sons; 2015.
REFERENCES
Appendix
Appendix 1.
- 1. Rue H, Martino S, Chopin N. Approximate Bayesian inference for latent Gaussian models by using integrated nested Laplace approximations. J R Stat Soc Series B Stat Methodol 2009;71:319-392.Article
- 2. Martino S, Rue H. Implementing approximate Bayesian inference using integrated nested Laplace approximation: a manual for the INLA program; 2008 [cited 2017 Jun 20]. Available from: http://www.bias-project.org.uk/GMRFCourse/inla-program.pdf.
References
Figure & Data
References
Citations
Citations to this article as recorded by 

- Environments affect blood pressure in toddlers: The Japan Environment and Children’s Study
Keita Kanamori, Tomohisa Suzuki, Nozomi Tatsuta, Chiharu Ota, Michihiro Kamijima, Shin Yamazaki, Yukihiro Ohya, Reiko Kishi, Nobuo Yaegashi, Koichi Hashimoto, Chisato Mori, Shuichi Ito, Zentaro Yamagata, Hidekuni Inadera, Takeo Nakayama, Tomotaka Sobue, M
Pediatric Research.2024; 95(1): 367. CrossRef - Passive Smoking is Strongly Associated with Heart Disease in Hypertensive Workers: Analysis of the 2018 Indonesia Basic Health Research
Astridya Paramita, Lely Indrawati, Nailul Izza, Dwi Hapsari Tjandrarini, Pramita Andarwati, Zainul Khaqiqi Nantabah, Maxwell Landri Vers Malakauseya, Christiana Rialine Titaley
Asian Journal of Social Health and Behavior.2024; 7(1): 37. CrossRef - Sleep-related adverse events of smoking cessation drugs: A network meta-analysis of randomized controlled trials
Yubin Song, Yoon-A Park, Da Hoon Lee, Jeong Yee, Hye Sun Gwak
Psychiatry Research.2024; 335: 115874. CrossRef - Influence of lifestyle on stroke risk among adults over 65 years in northern China: A propensity score matched study
Qiang Zhou, Yanyan Zhao, Haiying Chen, Hongyu Sun, Yumei Sun, Jie Li, Huiyong Yu, Qian Zhao, ZhiYan Zhang
European Journal of Integrative Medicine.2023; 58: 102224. CrossRef - Smoke Exposure Reduces the Protective Effect of Physical Activity on Hypertension: Evidence from the National Health and Nutrition Examination Survey (NHANES) 2013–2018
Chen Li, Yiyi Wang, Shouyu Wang, Lei Huang
International Journal of Environmental Research and Public Health.2023; 20(3): 2532. CrossRef - The effects of cigarette smoking and alcohol drinking on salty taste preferences based on Korean Community Health Survey data
Jian Ma, Yeon-Kyung Lee
Nutrition Research and Practice.2023; 17(3): 487. CrossRef - Challenges of Second-hand Smoke: Are We Asking the Right Questions?
Akash Deep Sharma, Rashmi Raghavan, Suneela Garg, Pradeep Aggarwal, Surekha Kishore, Om Prakash Bera
Indian Journal of Community Health.2023; 35(1): 04. CrossRef - Cohort Profile: ChinaHEART (Health Evaluation And risk Reduction through nationwide Teamwork) Cohort
Runsi Wang, Yang Yang, Jiapeng Lu, Jianlan Cui, Wei Xu, Lijuan Song, Chaoqun Wu, Xiaoyan Zhang, Hao Dai, Hui Zhong, Binbin Jin, Wenyan He, Yan Zhang, Hao Yang, Yunfeng Wang, Xingyi Zhang, Xi Li, Shengshou Hu
International Journal of Epidemiology.2023; 52(5): e273. CrossRef - Shared Lifestyle-Related Risk Factors of Cardiovascular Disease and Cancer: Evidence for Joint Prevention
Farzad Masoudkabir, Noushin Mohammadifard, Arya Mani, Andrew Ignaszewski, Margot K. Davis, Golnaz Vaseghi, Marjan Mansourian, Christopher Franco, Carolyn Gotay, Nizal Sarrafzadegan, Francesco Giallauria
The Scientific World Journal.2023; 2023: 1. CrossRef - Examining the Association between Cigarette Smoking Quantity and Subjective Salt Taste Preference and Salt-Related Eating Behavior
Jian Ma, Yeon-Kyung Lee
Korean Journal of Family Medicine.2023; 44(6): 335. CrossRef - Smoking waterpipe, cigarette, and heart disease: a cross-sectional analysis of baseline data from the Kong Cohort Study in the South of Iran
Maryam Karimi Jaberi, Nahid Shahabi, Shokrollah Mohseni, Zahra Karimi Jaberi, Shahin Abbaszadeh, Faeghe Zarei, Sara Dadipoor
Journal of Ethnicity in Substance Abuse.2023; : 1. CrossRef - Clinical Pathway for Coronary Atherosclerosis in Patients Without Conventional Modifiable Risk Factors
Gemma A. Figtree, Stephen T. Vernon, Jason A. Harmer, Michael P. Gray, Clare Arnott, Eric Bachour, Giannie Barsha, David Brieger, Alex Brown, David S. Celermajer, Keith M. Channon, Nicholas W.S. Chew, James J.H. Chong, Clara K. Chow, Peter A. Cistulli, Pa
Journal of the American College of Cardiology.2023; 82(13): 1343. CrossRef - Cardiovascular comorbidities and their prognostic value in small cell lung cancer patients with chemoradiotherapy
Hanyang Liang, Tianjie Wang, Dong Liu, Hao Wang, Zhengqing Ba, Ying Xiao, Yilu Liu, Jiansong Yuan, Weixian Yang
Clinical and Translational Oncology.2023;[Epub] CrossRef - Association between periodontal condition and blood pressure is confounded by smoking
Emilia Ollikainen, Tuomas Saxlin, Tellervo Tervonen, Anna Liisa Suominen, Matti Knuuttila, Antti Jula, Pekka Ylöstalo
Acta Odontologica Scandinavica.2022; 80(6): 457. CrossRef - Adherence to the healthy lifestyle guideline in relation to the metabolic syndrome: Analyses from the 2013 and 2018 Indonesian national health surveys
Fathimah S. Sigit, Stella Trompet, Dicky L. Tahapary, Dante S. Harbuwono, Saskia le Cessie, Frits R. Rosendaal, Renée de Mutsert
Preventive Medicine Reports.2022; 27: 101806. CrossRef - Prevalence and Related Factors of White Coat Hypertension and Masked Hypertension in Shunde District, Southern China
Hailan Zhu, Haoxiao Zheng, Xiaoyan Liang, Chunyi Huang, Lichang Sun, Xiong Liu, Min Qiu, Weiyi Mai, Yuli Huang
Frontiers in Physiology.2022;[Epub] CrossRef - Angina Outcomes in Secondhand Smokers: Results from the National Health and Nutrition Examination Survey 2007–2018
Suzanne Chaar, Jeik Yoon, Joud Abdulkarim, José Villalobos, Jeanette Garcia, Humberto López Castillo
Avicenna Journal of Medicine.2022; 12(02): 073. CrossRef - Tabakrauch – assoziierte Erkrankungen
Christian J. Herold
Die Radiologie.2022; 62(9): 729. CrossRef - Association between smoking and hypertension under different PM2.5 and green space exposure: A nationwide cross-sectional study
Qihao Chen, Xuxi Ma, Yan Geng, Jingling Liao, Lu Ma
Frontiers in Public Health.2022;[Epub] CrossRef - Awareness of hazards due to tobacco among people aged
15 years and older in Chongqing, China, in 2020: A cross-sectional
analysis
Qiu Chen, Jia Nan Dai, Xiao Dan Chen, Tian Qin, Wei Yun Lai, Yang Wang
Tobacco Induced Diseases.2022; 20(December): 1. CrossRef - The Interaction between Occupational Stress and Smoking, Alcohol Drinking and BMI on Hypertension in Chinese Petrochemical Workers
Zhihui Gu, Yunting Qu, Hui Wu
International Journal of Environmental Research and Public Health.2022; 19(24): 16932. CrossRef - Secondhand smoke: An unintended public health concern
Suneela Garg, AkashDeep Sharma
Indian Journal of Community and Family Medicine.2022; 8(2): 81. CrossRef - Secondhand smoking and neurological disease: a meta-analysis of cohort studies
Wei Liu, Bin Wang, Yang Xiao, Dongming Wang, Weihong Chen
Reviews on Environmental Health.2021; 36(2): 271. CrossRef - Passive smoking exposure and the risk of hypertension among non-smoking adults: the 2015–2016 NHANES data
Onoja Matthew Akpa, Akinkunmi Paul Okekunle, Jeffery Osahon Asowata, Babatunde Adedokun
Clinical Hypertension.2021;[Epub] CrossRef - Cocaine Use and White Matter Hyperintensities in Homeless and Unstably Housed Women
Elise D. Riley, Felicia C. Chow, S. Andrew Josephson, Samantha E. Dilworth, Kara L. Lynch, Amanda N. Wade, Carl Braun, Christopher P. Hess
Journal of Stroke and Cerebrovascular Diseases.2021; 30(5): 105675. CrossRef - Developing and validating the Malay version instrument to assess knowledge, attitudes and practices regarding second-hand smoke in the workplace: a cross-sectional study in teaching hospital in Malaysia
Ikmal Rashiden, Nur Amani Natasha Ahmad Tajuddin, Anne Yee, Amer Siddiq Amer Nordin
Environmental Science and Pollution Research.2021; 28(32): 44557. CrossRef - The effects of community participation program on smoke-free homes in a suburban community of Thailand
Peeraya Suteerangkul, Sunee Lagampan, Surintorn Kalampakorn, Naruemon Auemaneekul
Tobacco Induced Diseases.2021; 19(May): 1. CrossRef - Relationship between Exposure to Cigarette Smoke in Houses and The Incidence of Hypertension in Housewives
Anugrah Lintang Indrawati, Santi Martini
Jurnal Berkala Epidemiologi.2021; 9(2): 175. CrossRef - Impacts of Cigarette Smoking Status on Metabolomic and Gut Microbiota Profile in Male Patients With Coronary Artery Disease: A Multi-Omics Study
Xiaomin Hu, Yue Fan, Hanyu Li, Ruilin Zhou, Xinyue Zhao, Yueshen Sun, Shuyang Zhang
Frontiers in Cardiovascular Medicine.2021;[Epub] CrossRef - Association Between Passive Smoking and Health Among Chinese Nurses: A Cross-Sectional Study
Chun-ling Xia, Shi-qi Xiao, Qi-jun Wu, Xin-ying Yu, Lin-lin Xing, Li Gai, Tian-hui Xia, Hui-ling Feng, Xin-ying Zhang, Ying Guo, Yi-wei Xu, Tong-tong Fu, Xiang-hong Sun, Ling Fan
Frontiers in Public Health.2021;[Epub] CrossRef - Dependência do tabaco e nível de monóxido de carbono em trabalhadores terceirizados
Nayara Pires Nadaleti, Jefferson Felipe Ribeiro, Poliana Martins Ferreira, Sérgio Valverde Marques dos Santos, Denismar Alves Nogueira, Adriana Olimpia Barbosa Felipe, Fábio De Souza Terra
Ciência, Cuidado e Saúde.2021;[Epub] CrossRef - Interactions between Prepregnancy Overweight and Passive Smoking for Macrosomia and Large for Gestational Age in Chinese Pregnant Women
Dingyu Cui, Wen Yang, Ping Shao, Jing Li, Peng Wang, Junhong Leng, Shuo Wang, Enqing Liu, Juliana C.N. Chan, Zhijie Yu, Gang Hu, Xilin Yang
Obesity Facts.2021; 14(5): 520. CrossRef - Passive Smoking Exposure in Living Environments Reduces Cognitive Function: A Prospective Cohort Study in Older Adults
Fan He, Tian Li, Junfen Lin, Fudong Li, Yujia Zhai, Tao Zhang, Xue Gu, Genming Zhao
International Journal of Environmental Research and Public Health.2020; 17(4): 1402. CrossRef - BMI modified the association of current smoking with the incidence of hypertension in Chinese population: a 22-year cohort study
Feifei Yao, Wenfeng Liu, Rencheng Zhao, Guangxiao Li, Xiaojuan Huang, Yongjie Chen
BMC Public Health.2020;[Epub] CrossRef - How Do Combustion and Non-Combustion Products Used Outdoors Affect Outdoor and Indoor Particulate Matter Levels? A Field Evaluation Near the Entrance of an Italian University Library
Vittoria Cammalleri, Daniela Marotta, Carmela Protano, Matteo Vitali, Paolo Villari, Maria Cattaruzza
International Journal of Environmental Research and Public Health.2020; 17(14): 5200. CrossRef - Household Air Pollution and Angina Pectoris in Low- and Middle-Income Countries: Cross-Sectional Evidence from the World Health Survey 2002–2003
Ishwar Tiwari, Raphael M. Herr, Adrian Loerbroks, Shelby S. Yamamoto
International Journal of Environmental Research and Public Health.2020; 17(16): 5802. CrossRef - Associations between Lifestyle Factors and Vitamin E Metabolites in the General Population
Leon G. Martens, Jiao Luo, Fleur L. Meulmeester, Nadia Ashrafi, Esther Winters van Eekelen, Renée de Mutsert, Dennis O. Mook-Kanamori, Frits R. Rosendaal, Ko Willems van Dijk, Kevin Mills, Raymond Noordam, Diana van Heemst
Antioxidants.2020; 9(12): 1280. CrossRef - The association of smoking and hypertension according to cotinine-verified smoking status in 25,150 Korean adults
Sung Hoon Kim, Ju Suk Lee
Clinical and Experimental Hypertension.2019; 41(5): 401. CrossRef - Effect of transcranial direct current stimulation on the number of smoked cigarettes in tobacco smokers
Faisal Alghamdi, Ahmed Alhussien, Meshal Alohali, Abdullah Alatawi, Tariq Almusned, Shirley Fecteau, Syed Shahid Habib, Shahid Bashir, Andrea Antal
PLOS ONE.2019; 14(2): e0212312. CrossRef - The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2019)
Satoshi Umemura, Hisatomi Arima, Shuji Arima, Kei Asayama, Yasuaki Dohi, Yoshitaka Hirooka, Takeshi Horio, Satoshi Hoshide, Shunya Ikeda, Toshihiko Ishimitsu, Masaaki Ito, Sadayoshi Ito, Yoshio Iwashima, Hisashi Kai, Kei Kamide, Yoshihiko Kanno, Naoki Kas
Hypertension Research.2019; 42(9): 1235. CrossRef - Smoke-Free Policies and 30-Day Readmission Rates for Chronic Obstructive Pulmonary Disease
Sericea Stallings-Smith, Hanadi Y. Hamadi, Breck N. Peterson, Emma J.I. Apatu, Aaron C. Spaulding
American Journal of Preventive Medicine.2019; 57(5): 621. CrossRef - Further Insights on Predictors of Environmental Tobacco Smoke Exposure during the Pediatric Age
Carmela Protano, Vittoria Cammalleri, Arianna Antonucci, Alexandra Sabina Ungureanu, Francesa Santilli, Stefano Martellucci, Vincenzo Mattei, Matteo Vitali
International Journal of Environmental Research and Public Health.2019; 16(21): 4062. CrossRef - Smoking cessation in cardiovascular diseases
Kalea Despoina, Ioannis Vogiatzis
British Journal of Cardiac Nursing.2018; 13(3): 116. CrossRef - An approach to reduce the regional gap of health equity : What factors influence walking practices between two districts by social ecological model?
Kang Ju Son, Hoon Jo, Chun-Bae Kim, Su Mi Kim, In Gi Min, In Deok Kong
Korean Journal of Health Education and Promotion.2018; 35(4): 35. CrossRef - The relation of passive smoking with cervical cancer
Benyu Su, Wen Qin, Feng Xue, Xiaomin Wei, Qiangdong Guan, Wenchong Jiang, Shue Wang, Mengmeng Xu, Sufang Yu
Medicine.2018; 97(46): e13061. CrossRef - Influence of environmental tobacco smoke on morphology and functions of cardiovascular system assessed using diagnostic imaging
Paweł Gać, Małgorzata Poręba, Krystyna Pawlas, Małgorzata Sobieszczańska, Rafał Poręba
Inhalation Toxicology.2017; 29(12-14): 518. CrossRef

 KSE
KSE
 PubReader
PubReader ePub Link
ePub Link Cite
Cite